Type 1 Diabetes Management

Internist
Type 1 Diabetes Management: Symptoms, Diagnosis, Treatment
Type 1 diabetes does not usually give you much time. Symptoms can build fast, and serious complications can follow if a doctor does not evaluate them early.
FAQs
Type 1 Diabetes Management FAQs
Please feel free to Send a Message or call us if your related question is not included here. we are happy to serve you.
Early signs usually include increased thirst, frequent urination, fatigue, hunger, blurred vision, and unexplained weight loss. In children, bedwetting after staying dry can also be a clue
Yes. Type 1 diabetes is often diagnosed in children and young adults, but it can develop at any age. In some adults, symptoms may be slower and need extra testing to confirm the type.
Insulin is the main treatment. Research and medical experts that people with type 1 diabetes need insulin to stay alive.
Based on the American Diabetes Association’s 2026 guidance, established type 1 diabetes does not currently have a cure. While teplizumab can help delay the onset of stage 3 disease in selected at-risk individuals, it is not a cure for type 1 diabetes once the disease has been diagnosed.
Home care means keeping insulin and supplies organized, Online visits regularly, monitoring glucose, treating lows quickly, knowing when ketones matter, and having a sick-day and emergency plan.
For most people with diabetes, blood sugar below 70 mg/dL is considered low and should be treated.
Some patients notice mild changes at first. Others get sick very quickly. A child may start asking for water all day. An adult may lose weight without trying, feel exhausted, or need to urinate far more often than usual. Because of that, early recognition matters.
Type 1 diabetes develops when the immune system attacks the cells in the pancreas that make insulin. As insulin levels fall, glucose stays in the blood instead of moving into the cells for energy. As a result, blood sugar rises, and the body starts to struggle.
For patients and families, good type 1 diabetes management starts with three things: spotting the warning signs, getting the right diagnosis, and beginning a safe treatment plan without delay.
What Type 1 Diabetes Is
Type 1 diabetes is an autoimmune disease. In this condition, the immune system attacks the beta cells in the pancreas. Those cells make insulin. When the body loses them, insulin production drops and blood sugar rises.
Without enough insulin, glucose cannot enter the cells properly. Instead, it builds up in the bloodstream. Meanwhile, the body’s tissues still need fuel, so patients often feel weak, thirsty, hungry, or mentally foggy.
What causes type 1 diabetes?
The short answer is autoimmunity. The more honest answer is that doctors know the immune system attacks beta cells, but they still do not know every reason why that process starts in a given person. Genes matter. Family history matters. Environmental triggers may matter too.
What deserves emphasis is what does not cause type 1 diabetes. Diet and lifestyle habits do not cause it. A child did not get it from eating sugar. A thin adult did not “earn” it by doing something wrong. That misconception is common and unhelpful.
If a parent or sibling has type 1 diabetes, risk is higher, and family members may be offered screening for diabetes-related autoantibodies. In the U.S., TrialNet offers testing for some relatives of people with type 1 diabetes, even if they have no symptoms.
How type 1 diabetes differs from type 2 diabetes
Type 1 diabetes and type 2 diabetes are not the same condition. In type 1 diabetes, the main problem is insulin loss caused by autoimmunity. In type 2 diabetes, the body usually still makes insulin, but it does not use it well. That problem is called insulin resistance.
Although both conditions can raise blood sugar, doctors do not manage them the same way. For that reason, patients need the right diagnosis from the start.
Who can develop type 1 diabetes?
Type 1 diabetes is often diagnosed in children and young adults, but it can develop at any age. Adults can develop it too, and in some cases, the diagnosis is delayed because the symptoms are initially mistaken for another form of diabetes.
What Causes Type 1 Diabetes
Doctors know the core cause of type 1 diabetes: autoimmunity. The immune system wrongly attacks the insulin-producing cells in the pancreas. However, medicine still does not know every reason this process starts in one person and not another.
Genes may raise the risk. Family history may matter too. In addition, researchers continue to study environmental triggers that may help start the disease process.
Genetics and family history
Family history can raise risk, although many people diagnosed with type 1 diabetes do not have a close relative with the condition. If a parent or sibling has type 1 diabetes, risk is higher than in the general population.
Environmental triggers
Researchers continue to study which environmental triggers may contribute to the autoimmune process. The exact trigger is not always identifiable in an individual patient, which is why families are often left asking “why did this happen?” without getting a simple answer.
What does not cause type 1 diabetes
This point needs to be clear because patients hear harmful myths all the time: type 1 diabetes is not caused by eating sugar, by being inactive, or by “bad habits.” CDC says the exact cause is not fully known, but diet and lifestyle habits are not the reason type 1 diabetes develops.
Type 1 Childhood Diabetes Symptoms and Adult Warning Signs
Symptoms of type 1 diabetes often appear quickly. In some patients, the change happens over a few weeks. In others, it becomes obvious within days. Either way, the pattern deserves attention.
Common symptoms include:
- Unusual thirst
- Frequent urination
- Increased hunger
- Fatigue
- Blurred vision
- Unexplained weight loss
- Nausea or stomach discomfort in some cases
What type 1 diabetes management really means
This is where many people get overwhelmed, especially after being newly diagnosed with diabetes. They imagine treatment as “take insulin and avoid sugar.” Real type 1 diabetes management is more structured than that, but it is also more workable than many people fear.
At the center of the plan are four moving parts:
- Insulin
- Glucose monitoring
- Food and activity decisions
- Ongoing adjustment with a care team
The goal is not perfection. The goal is safer, steadier glucose, fewer emergencies, and lower long-term risk. NIDDK recommends building a diabetes care plan with your health care team rather than trying to improvise day by day.
Type 1 childhood diabetes symptoms
Parents often search for type 1 childhood diabetes symptoms because the first signs can look ordinary. A child may drink more water, ask for the bathroom more often, or seem tired for no clear reason. Still, when several of these signs appear together, families should not ignore them.
If a child also loses weight, wets the bed again, or seems unusually weak, a medical evaluation should happen quickly.
When symptoms become urgent
Sometimes the problem becomes urgent very quickly. If vomiting, stomach pain, rapid breathing, fruity-smelling breath, confusion, or severe tiredness develop, diabetic ketoacidosis may be the cause.
This condition, often called DKA, is a medical emergency. It happens when the body does not have enough insulin and starts producing high levels of ketones. At that point, the patient needs urgent medical care.
How Type 1 Diabetes Is Diagnosed
Doctors diagnose type 1 diabetes with blood tests. First, they confirm that diabetes is present. Then, if needed, they look more closely to determine which type of diabetes the patient has.
That second step matters. Some adults with type 1 diabetes are first labeled as having type 2 diabetes. However, the treatment plan changes significantly once the true diagnosis becomes clear.
Blood tests used to diagnose diabetes
NIDDK lists the main diagnostic tests as:
- A1C
- Fasting plasma glucose
- Random plasma glucose
- Oral glucose tolerance test
According to NIDDK, diabetes can be diagnosed at:
- A1C of 6.5% or higher
- Fasting plasma glucose of 126 mg/dL or higher
- 2-Hour oral glucose tolerance test result of 200 mg/dL or higher
- Random plasma glucose of 200 mg/dL or higher when symptoms are present
How doctors confirm it is type 1 diabetes
A high glucose result confirms diabetes, but it does not always identify the subtype. When the clinical picture is unclear, clinicians may use autoantibody testing, and sometimes other lab evaluations, to help confirm type 1 diabetes. NIDDK notes that certain autoantibodies in the blood can support the diagnosis of type 1 diabetes.
This matters in real practice. Adults with new diabetes are sometimes assumed to have type 2 diabetes when they actually have autoimmune diabetes and need insulin-based treatment.
Type 1 Diabetes Management: What Treatment Looks Like in Practice
In real life, type 1 diabetes management involves more than one task. Patients need insulin, blood sugar monitoring, meal planning, activity awareness, and regular follow-up. In other words, treatment is not a single prescription. It is an ongoing medical plan.
The goal is not perfection. Instead, the goal is safer blood sugar patterns, fewer emergencies, and better long-term health.
Insulin therapy for type 1 diabetes
Insulin therapy for type 1 diabetes is the foundation of treatment. Patients need insulin every day. Usually, the plan includes a background insulin component and a mealtime or correction insulin component.
Doctors may prescribe insulin by syringe, pen, or pump. The best option depends on the patient’s age, routine, glucose trends, and comfort with devices. Because of that, treatment should always be personalized.
Type 1 diabetes medication
When patients search for type 1 diabetes medication, the most important answer is still insulin. Other supportive medications may be considered in selected cases, but insulin remains the essential treatment. Any care plan for type 1 diabetes that does not address insulin properly is incomplete.
Glucose monitoring and diabetes technology
Effective treatment also depends on regular glucose monitoring. CDC says blood sugar can be checked with a blood glucose meter or a continuous glucose monitor, and a CGM measures glucose every few minutes.
For many patients, CGM technology improves safety and day-to-day decision-making because it shows trends, not just isolated readings. CDC specifically notes that CGMs are especially useful for people with type 1 diabetes.
Type 1 Diabetes Management Between Visits
Good diabetes care does not happen only during appointments. It continues at home, at school, at work, during exercise, and while traveling. For that reason, patients need a plan that works in real life, not just on paper.
Food, meals, and daily structure
Patients with type 1 diabetes need a practical food plan. They do not need vague advice like “just avoid sugar.” Instead, they need to understand how meals, carbohydrates, timing, and insulin work together.
That approach is more useful because it helps patients make daily decisions with less confusion.
Type 1 diabetes insulin sensitivity
Type 1 diabetes insulin sensitivity can change from day to day. Exercise may lower blood sugar. Illness, stress, and poor sleep may raise it. As a result, the same insulin dose may not act the same way every day.
This is one reason diabetes care requires ongoing review. Patients are not failing when patterns change. Rather, the body is responding to different conditions.
Newly diagnosed diabetes
A patient with newly diagnosed diabetes often receives a large amount of information all at once. That can feel overwhelming. So, the first goal should be safety, not perfection.
Patients should first learn how to take insulin, check blood sugar, recognize highs and lows, and know when to call the doctor. After that, they can build confidence step by step.
Type 1 Diabetes High Blood Sugar Levels, Lows, and Sick Days
This is where daily diabetes care becomes very practical. Patients need to know what high blood sugar feels like, how to treat low blood sugar, and what changes during illness. Otherwise, small problems can become medical emergencies.
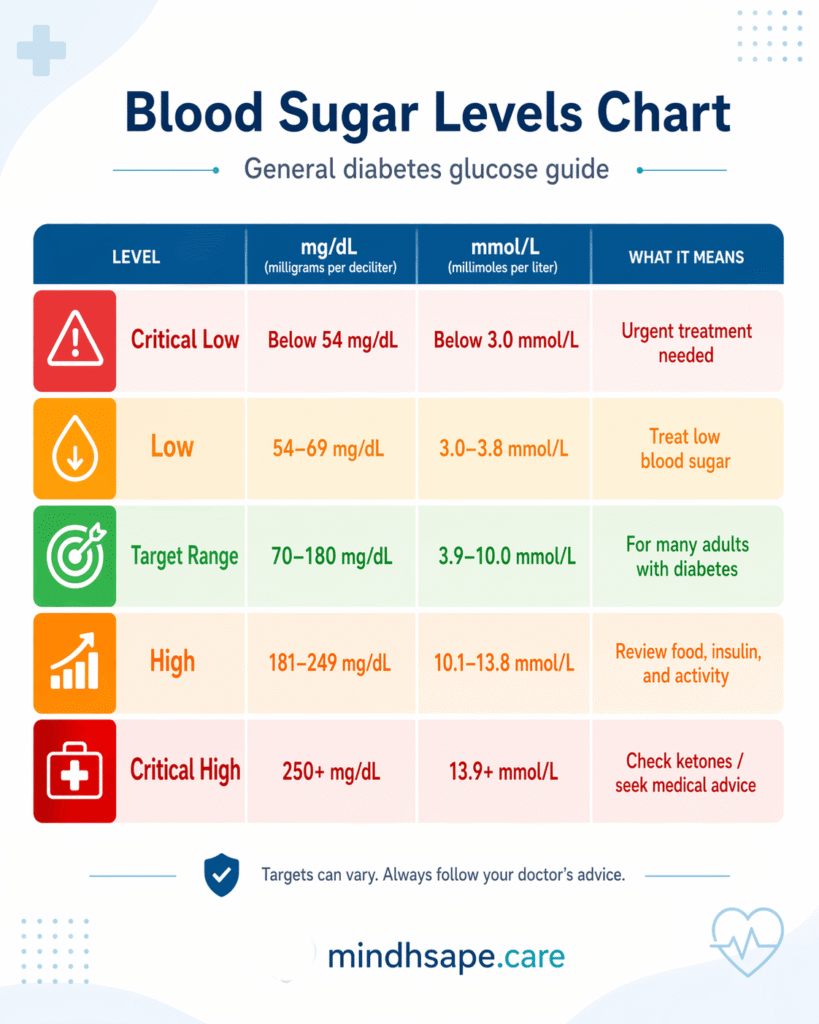
Type 1 diabetes high blood sugar levels
Type 1 diabetes high blood sugar levels can cause thirst, fatigue, frequent urination, blurred vision, and difficulty concentrating. NIDDK notes that for many people with diabetes, glucose above 180 mg/dL is considered high, although targets should be individualized with the treating clinician.
Repeated highs are not something to normalize. They should lead to a review of insulin timing, dosing, meals, illness, stress, and device function.
When ketones matter
Ketones matter most when blood sugar is high and the patient feels sick. They can signal that the body does not have enough insulin. If vomiting, dehydration, or rapid worsening also appears, the risk becomes much more serious.
Because of that, patients should follow their sick-day plan closely and seek medical advice early when ketones rise.
Low blood sugar and the 15-15 rule
Low blood sugar needs fast action. For many mild episodes, patients can use the 15-15 rule: take 15 grams of carbohydrates, wait 15 minutes, and recheck the blood sugar.
Even so, severe lows need urgent help. Family members should know what symptoms to watch for and when emergency treatment is necessary.
How to Care for a Diabetic Patient at Home
Families often search how to care for a diabetic patient at home soon after diagnosis. That makes sense. The condition affects daily routines right away.
Good home care should feel organized, calm, and practical. Above all, it should make it easier to follow the treatment plan safely.
Daily home care basics
A safe home setup usually includes:
- Insulin and backup supplies in an organized place, with a clear monitoring routine
- Fast-acting carbohydrates available for lows
- A ketone-testing plan if the care team recommends one
- Written sick-day instructions
- Emergency contact information that is easy to access
Help with diabetes meds
Some patients need help with diabetes meds, especially in the early weeks. They may need help with refill timing, insulin schedules, device use, or insurance approvals. That is normal.
When the plan feels unclear, patients should contact their doctor, diabetes educator, or pharmacist early. Doing so often prevents bigger problems later.
School, work, and daily functioning
For children, school planning matters. CDC recommends making a diabetes management plan with school staff and coordinating care so the child can stay safe and participate fully.
For adults, the same principle applies in a different setting: work routines, meal timing, exercise, commuting, and illness all need to be accounted for in the care plan.
Is There a Type 1 Diabetes Cure?
Patients ask about a type 1 diabetes cure all the time. The answer should be clear and direct: there is no cure for established type 1 diabetes right now. Even though treatment has improved, patients still need lifelong medical care and insulin-based management after diagnosis.
What has changed is the prevention and delay side of care. The FDA approved teplizumab-mzwv to delay the onset of stage 3 type 1 diabetes in adults and children age 8 and older with stage 2 disease. That is important progress, but it is not a cure for patients who already have symptomatic type 1 diabetes.
This distinction matters on a medical service website. Patients need hope, but they also need accuracy.
When to Seek Medical Help Right Away
Some symptoms need urgent medical attention. Patients should not try to manage severe warning signs at home for too long.
Patients should seek urgent medical care if they have:
- Vomiting with high blood sugar, abdominal pain, plus dehydration
- Rapid or labored breathing
- Confusion
- Fainting
- Suspected DKA
- Inability to keep fluids down
- Severe low blood sugar that cannot be safely treated at home
The right message is simple: if symptoms are escalating, do not rely on guesswork.
Final Thoughts on Type 1 Diabetes Management
Strong type 1 diabetes management starts with the right diagnosis. After that, patients need a clear insulin plan, regular monitoring, and dependable medical follow-up.
The daily work is real. Still, patients do much better when they have a clear care plan and access to an experienced clinical team. Step by step, good treatment leads to safer numbers, fewer emergencies, and more confidence.
Ready to Get Support?
Book an appointment with a licensed doctor for evaluation, diagnosis review, and a personalized diabetes care plan.
If you have already been diagnosed, our clinical team can help you understand treatment options, insulin routines, blood sugar patterns, and next-step management.
A caring note from MindShape Care
This article is for education only and is not a diagnosis. If your symptoms feel severe, urgent, or unsafe, please seek immediate emergency or crisis support.
This article was reviewed and written with insights from the Medical team at Medically reviewed by licensed clinicians at mindhsape.care. in the USA — experienced healthcare professionals specializing in anxiety, depression, chronic kidney disease, all types of diabetes, hair loss, hormonal health, hyperlipidemia, hypertension, low testosterone, nutrition management, obesity, obstructive sleep apnea, PCOS, and infertility, and patient wellness. Learn more about our board-certified doctors and treatment experts who contribute to our educational blogs and patient support programs.
Recent Blogs
Learn more about Virtual Healthcare and Treatments
Why You Can Rely on Us?
At Mindshape Clinic, we are committed to providing clear and trustworthy health information that you can rely on.
Reliable Information – Every article is based on credible sources.
Expert Review – Content is carefully checked before publishing.
Up to Date – We keep information current with the latest insights.
Clarity First – Our goal is to make knowledge simple and accessible.