Prediabetes Management Online

Internist
Prediabetes Management: Causes, Symptoms, Diagnosis, and Treatment
Prediabetes does not sound urgent. However, that is exactly why many patients underestimate it.
The name can make it feel mild or easy to ignore. In reality, blood sugar is already running higher than normal, and the body is starting to struggle with glucose control.
FAQs
Prediabetes Management FAQs
Please feel free to Send a Message or call us if your related question is not included here. we are happy to serve you.
Yes, prediabetes is often reversible. According to CDC and NIDDK clinical data, losing 5% to 7% of your body weight and engaging in 150 minutes of weekly physical activity can reduce the risk of progressing to type 2 diabetes by 58%. Consistency in diet and weight management is the primary key to returning blood sugar to normal levels.
The official clinical range for prediabetes is an A1C of 5.7% to 6.4%. This blood test measures your average glucose levels over the past three months. Results below 5.7% are considered normal, while results of 6.5% or higher indicate a diagnosis of type 2 diabetes.
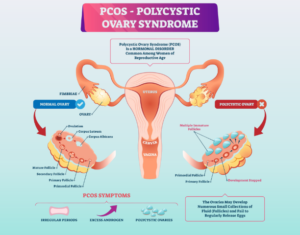
Most women with prediabetes experience no obvious symptoms. However, those with Polycystic Ovary Syndrome (PCOS) or a history of gestational diabetes are at significantly higher risk. Warning signs may include darkened skin in body creases (acanthosis nigricans), increased fatigue, and irregular menstrual cycles linked to insulin resistance.
While you can see significant improvements in your blood sugar within 90 days, "reversing" prediabetes depends on the individual. A1C reflects a 3-month average, so lifestyle changes made today will take a full cycle to show in your labs. Focus on sustainable calorie reduction rather than "crash" plans that NIDDK warns are rarely effective long-term.
The choice depends on your specific metabolic profile. Metformin has the most robust long-term data for diabetes prevention, especially in patients under age 60 with a BMI over 30. GLP-1 medications like Ozempic may be more beneficial for patients who require significant weight loss to manage their metabolic risk. This decision requires a clinician-guided evaluation.
There is no "single worst" food, but sugar-sweetened beverages (sodas, sweetened teas, and energy drinks) are the primary contributors to rapid blood sugar spikes. These provide "liquid calories" without fiber or protein, leading to increased insulin resistance. Replacing these with water or unsweetened alternatives is the fastest dietary shift you can make.
Generally, prediabetes does not cause abdominal pain. If you are experiencing stomach pain alongside high blood sugar, it may be a sign of a more serious condition like Diabetic Ketoacidosis (DKA) or severe insulin resistance. If pain persists, you should seek a medical evaluation to rule out gastrointestinal or metabolic emergencies.
That does not mean everyone with prediabetes will develop type 2 diabetes. It does mean the risk is real. NIDDK says people with prediabetes have a high chance of developing type 2 diabetes within 5 to 10 years. The good news is that there is a clear window for action. Lifestyle change, weight management, physical activity, and, in some cases, medication can delay or prevent type 2 diabetes.
For a clinic website, this topic should do more than define the condition. It should help patients understand what prediabetes is, what the prediabetes range means, whether symptoms matter, when A1C becomes concerning, what a prediabetes diet actually looks like, and where metformin for prediabetes fits. It should also reflect how a licensed medical team can support patients online with monitoring, goal-setting, and treatment decisions.
Prediabetes Management Starts With Understanding Prediabetes
Prediabetes is a state in which blood sugar is higher than normal but not yet high enough for a diabetes diagnosis. CDC says before developing type 2 diabetes, most people have prediabetes. NIDDK describes it as an intermediate stage in the development of type 2 diabetes.
What is prediabetes?
If you are asking what prediabetes is, the simplest answer is this: your body is already showing signs that it is not handling glucose well. In many patients, that starts with insulin resistance. NIDDK explains that insulin resistance means cells in the muscles, fat, and liver do not respond well to insulin. Over time, the pancreas may not make enough insulin to keep up, and blood glucose rises into the prediabetes range.
That matters because prediabetes is not just a lab technicality. It raises the risk of type 2 diabetes, heart disease, and stroke. CDC highlights all three as major concerns tied to prediabetes.
Why Early Prediabetes Management Matters
Early action matters because prediabetes can often improve before diabetes becomes established. Therefore, patients who understand their numbers early have a better chance to lower risk with realistic changes that last.
Prediabetes vs diabetes
The difference between prediabetes vs diabetes comes down to blood sugar thresholds and disease stage. In prediabetes, levels are elevated but below the diabetes cutoff. In diabetes, glucose levels are high enough to meet diagnostic criteria for the disease. That may sound like a small distinction, but it creates a big difference in treatment urgency, long-term risk, and the chance to turn things around before full diabetes develops.
So prediabetes is not “nothing.” It is the stage where prevention still has real power.
What Causes Prediabetes
Insulin resistance and risk factors
The main biological driver of prediabetes is insulin resistance. NIDDK says the body’s cells stop responding well to insulin, so glucose has a harder time moving from the bloodstream into the cells. As that problem builds, blood sugar rises.
Risk factors also matter. Risk is higher if a person is overweight, age 45 or older, physically active less than three times a week, has a parent or sibling with type 2 diabetes, had gestational diabetes, gave birth to a baby weighing more than 9 pounds, or has PCOS. NIDDK adds that overweight or obesity and other type 2 diabetes risk factors make prediabetes more likely.
The root cause of prediabetes
Patients often ask about the “real” cause, hoping for one culprit. Usually there is not just one. The root cause of prediabetes is often a mix of insulin resistance, excess body weight, genetics, low activity, sleep and metabolic health, and in some patients, hormonal or pregnancy-related history. That is why a smart treatment plan does not rely on one food rule or one supplement. It looks at the whole pattern.
Prediabetes Symptoms
Symptoms of prediabetes
Most people expect symptoms. That is understandable. But prediabetes often stays quiet.
There are usually no signs when you have prediabetes. People with insulin resistance and prediabetes usually have no symptoms.
That means the phrase prediabetes symptoms can be misleading. Many patients have no clear symptoms at all. Others may start to show signs more typical of higher blood sugar, especially as they move closer to diabetes. High blood glucose can cause tiredness, thirst, blurry vision, and urinating too often. Those are more classic hyperglycemia symptoms than specific “prediabetes only” symptoms, but they matter if they start showing up.
Acanthosis nigricans, or darkened skin in body creases, can also be a clue to insulin resistance in some patients. According to the medical research department of the CDC, acanthosis nigricans is a sign seen in people with PCOS, a condition linked to insulin resistance and higher diabetes risk.
Symptoms of prediabetes in females
The phrase symptoms of prediabetes in females gets searched often, but the core answer is the same: most women with prediabetes still have no obvious symptoms. That said, women with PCOS deserve special attention because identifies PCOS as a risk factor for prediabetes and type 2 diabetes. If a woman has PCOS, weight gain, acanthosis nigricans, irregular periods, or a strong family history of diabetes, testing is worth discussing early.
For a clinic website, the safest clinical message is this: do not wait for symptoms before getting tested if you have risk factors.
Prediabetes Diagnosis
Good Prediabetes Management starts with a correct diagnosis. Doctors diagnose prediabetes with blood tests. NIDDK says the three recommended ways to identify or diagnose prediabetes are the A1C test, fasting plasma glucose, and the 2-hour oral glucose tolerance test.
Prediabetes range and A1C for prediabetes
The prediabetes range is important because many patients see an abnormal result but do not know how to interpret it.
NIDDK states that any of the following confirm prediabetes:
- A1C 5.7% to 6.4%
- Fasting plasma glucose 100 to 125 mg/dL
- 2-hour OGTT 140 to 199 mg/dL
That is the official a1c prediabetes range and also the hba1c prediabetes range. If you are searching what is prediabetes A1C or a1c for prediabetes, the answer is the same: 5.7% to 6.4%.
What is prediabetes A1C?
A1C reflects the average blood glucose level over about three months. NIDDK explains that the A1C test gives information about average blood glucose over the past 3 months and can be used to diagnose both type 2 diabetes and prediabetes.
That makes A1C useful because it reflects a pattern, not just one moment. Still, NIDDK also notes that in some health conditions, the A1C test may miss prediabetes, so doctors may use fasting glucose or an OGTT when suspicion remains high.
Prediabetes ICD-10
If you work with claims, forms, or charting, the usual prediabetes ICD-10 code is R73.03. CMS materials list R73.03 as the code for prediabetes.
That is a technical detail, but patients sometimes search it because they see it on paperwork and want to know what it means.
Prediabetes Management Online: What Modern Care Includes
For a medical service provider, Prediabetes Management should not sound like “eat better and check back later.” Modern care is more structured than that.
With prediabetes should be counseled on weight loss, healthy food choices, and physical activity, and clinicians should consider referral to a structured lifestyle intervention such as the National Diabetes Prevention Program. National DPP focuses on calorie reduction, behavior change, and at least 150 minutes of physical activity a week.
Prediabetes Management with lifestyle change
Lifestyle change remains the first and strongest treatment for most patients with prediabetes. The original Diabetes Prevention Program showed that structured lifestyle change reduced diabetes risk by 58%. A 2025 review of the DPP and its follow-up confirmed that lifestyle intervention reduced diabetes development by 58% after 2.8 years, while metformin reduced it by 31% compared with placebo.
That does not make medication unimportant. It does show why lifestyle treatment stays at the center.
Blood sugar, blood pressure, and cholesterol
This is where many patients need a reset. Good diabetes care is not just about glucose. NIDDK says that managing blood glucose, blood pressure, and cholesterol is central to lowering the chances of heart attack, stroke, kidney disease, blindness, and amputations. That is why treatment plans often include blood pressure medicine, statins, kidney protection, or smoking cessation support in addition to glucose-lowering medication.
Prediabetes Management with weight loss and exercise
If you are asking how to control prediabetes, how to fix prediabetes, or how to get out of prediabetes, the most evidence-based starting point is modest weight loss plus consistent physical activity.
Losing 5% to 7% of body weight and getting at least 150 minutes a week of brisk walking or similar activity can lower the risk of type 2 diabetes substantially. The NIH-funded DPP showed that losing 5% to 7% of starting weight helped reduce the chance of developing the disease. ADA’s 2026 obesity prevention standards also state that in people with prediabetes, 5% to 7% weight loss reduces progression to diabetes, and greater weight loss produces additional benefits.
So when people search how to reverse prediabetes in 3 months or how to reverse prediabetes fast, the honest clinical answer is this: some patients can improve labs quickly, but the safest path is not a crash plan. It is a structured plan that improves diet quality, increases activity, and supports weight loss that can actually be maintained. NIDDK specifically warns that many popular “quick fix” weight-loss plans have not been proven to work long term or prevent type 2 diabetes.
Follow-up and repeat testing
If tests show you have prediabetes, you should be tested for type 2 diabetes every year. If you have risk factors but do not have prediabetes yet, retesting at least every 3 years is reasonable.
That is where online management can help. Patients often do better when they have regular check-ins, weight tracking, A1C follow-up, and practical coaching rather than one lecture and a long gap in care.
Prediabetes Diet
A strong Prediabetes Management plan includes practical food choices. However, patients do not need a crash diet. Instead, they need meals they can repeat, portions they can manage, and routines they can keep. That is what makes the plan work over time.
Diet for prediabetes
A prediabetes diet should be realistic, not punishing.
NIDDK says healthy living for insulin resistance and prediabetes includes consuming healthy foods and drinks, being physically active, managing weight, and getting enough sleep. CDC’s general healthy eating guidance emphasizes vegetables, fruits, whole grains, protein foods, and healthier fats, with attention to portion size and meal pattern.
So a strong diet for prediabetes usually includes:
- More vegetables and high-fiber foods
- More beans, lentils, eggs, yogurt, fish, chicken, tofu, and other protein sources
- Better carbohydrate quality rather than endless carbohydrate fear
- Fewer sugar-sweetened drinks
- Fewer ultra-refined snack foods eaten mindlessly
- More consistent portions and routines.
Foods to limit
Patients often ask, what foods should a prediabetic avoid? The better answer is not a rigid ban list. It is a pattern shift.
Limit frequent sugary drinks, oversized desserts, and refined carbohydrates that are easy to overeat and do not offer much fiber or fullness. NIDDK and CDC both support a reduced-calorie, healthier eating pattern aimed at sustainable weight loss and better glucose control.
That is also the best way to answer overly simple questions like what is the #1 worst food for your blood sugar? There is no universal single villain. In practice, sugar-sweetened drinks and large portions of refined carbohydrates are often the least helpful pattern for many patients.
Snack and breakfast questions
Patients also ask very specific questions because they want practical help.
-Are eggs ok for prediabetes?
Yes, eggs can fit into a prediabetes meal plan. They provide protein and can support a more balanced breakfast when paired with fiber-rich foods. That fits with general healthy eating guidance from CDC and NIDDK, which emphasizes nutrient-dense foods and balanced eating rather than blanket avoidance of whole foods.
-What is the best toast for a diabetic or prediabetic patient?
Usually a higher-fiber, less refined bread is a better choice than white toast, especially when paired with protein or healthy fat. The bigger issue is the full meal pattern, not just one slice of bread. That approach aligns with CDC’s and NIDDK’s broader guidance on healthier food choices and portion awareness.
-What is the number one snack to lower blood sugar?
There is no single magic snack that “lowers” blood sugar on command. The better strategy is to choose snacks that are less likely to spike it: for example, protein plus fiber, such as nuts, plain yogurt, hummus with vegetables, or apple slices with peanut butter. That is a practical inference from evidence-based healthy eating principles, not a standalone medical rule.
Metformin for Prediabetes
For most patients, lifestyle change comes first. However, Prediabetes Management may also include medication in selected higher-risk cases. That is where metformin fits. It is not the right choice for everyone, but it can help some patients lower diabetes risk.
When metformin prediabetes treatment may fit
Metformin for prediabetes is not the first step for everyone, but it does have a role.
NIDDK says clinicians should consider metformin for patients under age 60 with prediabetes plus other risk factors, such as A1C above 6%, hypertension, low HDL cholesterol, elevated triglycerides, family history of diabetes in a first-degree relative, and obesity with BMI 30 or greater. NIDDK also says metformin worked best in the DPP for women with a history of gestational diabetes, younger adults, and people with obesity. ADA’s 2026 prevention standards say metformin has the most robust efficacy and safety data as a pharmacologic therapy for diabetes prevention among people with prediabetes.
So if you are searching metformin prediabetes or metformin for prediabetes, the honest answer is: yes, it can be appropriate, but usually for selected higher-risk patients rather than automatically for everyone.
Metformin vs newer weight-loss medications
Patients now also ask about newer medication options, especially GLP-1 drugs such as semaglutide. For obesity treatment, semaglutide and other newer weight-management medicines can help some patients lose enough weight to improve metabolic risk. NIDDK notes that semaglutide was approved for obesity treatment and that weight-loss medicines can be helpful in some cases for people with insulin resistance or prediabetes.
So, which is better for prediabetes, Ozempic or metformin?
There is no single winner for every patient. Metformin has stronger direct prevention data in prediabetes. GLP-1-based medicines may be more helpful in selected patients whose main issue is overweight or obesity and who need substantial weight loss. Choice depends on goals, access, side effects, cost, and the full medical picture. That is why this decision belongs in a clinician-guided conversation, not a social media poll.
How to Reverse Prediabetes Fast and Safely
The phrase “how to reverse prediabetes fast” gets searched all the time. Still, fast is not the most useful goal. A better goal is steady improvement that lasts. In practice, that means weight loss, better food quality, more activity, and repeat lab follow-up.
How to get out of prediabetes
If your goal is how to get out of prediabetes or how to bring A1C down naturally, the most evidence-based plan looks like this:
- Lose 5% to 7% of body weight if you have overweight
- Reach 150 minutes a week of moderate activity
- Improve diet quality and portion control
- Get follow-up labs instead of guessing
- Consider medication if your risk is higher or progress stalls.
That is not flashy advice. It is the advice that actually has long-term data behind it.
How much weight do I need to lose to reverse prediabetes?
CDC gives the clearest practical benchmark: 5% to 7% of body weight. For a 200-pound person, that is about 10 to 14 pounds. NIDDK gives the same general range from the DPP research. ADA’s 2026 standards confirm that 5% to 7% weight loss reduces progression to diabetes, with greater weight loss bringing more benefit.
How much can A1C drop in 3 months?
There is no single guaranteed number. A1C reflects about three months of blood sugar trends, so meaningful improvement can happen in that window, but the size of the drop depends on where you start, how much weight you lose, what changes you make, and whether medication is involved. NIDDK explains what the A1C measures, while DPP-based data support the idea that structured lifestyle intervention can meaningfully reduce diabetes risk and improve glycemia. The safest clinical framing is: improvement in 3 months is possible, but individual results vary.
Final Thoughts on Prediabetes Management
Good Prediabetes Management is not about fear. It is about timing.
Prediabetes is the moment when abnormal blood sugar has appeared, but there is still a strong chance to prevent or delay type 2 diabetes. Diagnosis depends on clear blood-test thresholds. Symptoms are often absent. Treatment starts with lifestyle change, supported by weight loss, physical activity, and healthier eating. In selected high-risk patients, metformin may also help.
For a clinic website, the message should be practical: do not wait until diabetes becomes obvious. Get tested, understand the numbers, and build a plan you can actually keep. That is where prevention becomes real.
Get online Prediabetes management?
Book an online appointment with a licensed doctor for prediabetes evaluation, A1C review, lifestyle guidance, and a personalized prevention plan.
A caring note from MindShape Care
This article is for education only and is not a diagnosis. If your symptoms feel severe, urgent, or unsafe, please seek immediate emergency or crisis support.
This article was reviewed and written with insights from the Medical team at Medically reviewed by licensed clinicians at mindhsape.care. in the USA — experienced healthcare professionals specializing in anxiety, depression, chronic kidney disease, all types of diabetes, hair loss, hormonal health, hyperlipidemia, hypertension, low testosterone, nutrition management, obesity, obstructive sleep apnea, PCOS, and infertility, and patient wellness. Learn more about our board-certified doctors and treatment experts who contribute to our educational blogs and patient support programs.
Why You Can Rely on Us?
At Mindshape Clinic, we are committed to providing clear and trustworthy health information that you can rely on.
Reliable Information – Every article is based on credible sources.
Expert Review – Content is carefully checked before publishing.
Up to Date – We keep information current with the latest insights.
Clarity First – Our goal is to make knowledge simple and accessible.