Type 2 Diabetes Management

Internist
Type 1 Diabetes Management: Symptoms, Diagnosis, Treatment
Type 2 diabetes usually does not arrive with the drama of a medical emergency. More often, it develops quietly. Blood sugar creeps up. Energy drops. Vision blurs. Weight, hunger, and bathroom habits change. Sometimes there are no obvious symptoms at all.
FAQs
Type 2 Diabetes Management FAQs
Please feel free to Send a Message or call us if your related question is not included here. we are happy to serve you.
The most common treatments are healthy eating, increased physical activity, weight management, blood sugar monitoring when needed, and medication. Metformin is a common starting medication, but many patients may also need GLP-1 medicines, SGLT2 inhibitors, or other drugs depending on weight, kidney disease, heart disease, and blood sugar levels.
In practical terms, a newly diagnosed patient should confirm the diagnosis, review A1C and other labs, begin a realistic food and activity plan, discuss medication, and learn what blood sugar targets to aim for. Patients also need a plan for follow-up, eye care, kidney checks, blood pressure, and cholesterol.
Start with a balanced meal pattern built around vegetables, protein, high-fiber carbohydrates, and unsweetened drinks. CDC recommends eating healthy foods in the right amounts at the right times and working with a dietitian or diabetes educator on meal planning.
For most people, below 70 mg/dL is too low and above 180 mg/dL is too high. The situation becomes more urgent when blood sugar stays very high, especially with illness. CDC says sick patients with diabetes should check ketones if blood sugar is 250 mg/dL or above, and urgent care is needed if blood sugar stays 300 mg/dL or higher with DKA symptoms.
Historically, metformin has been the first-line medication for type 2 diabetes. That is still true in many cases. However, ADA’s current standards support more individualized first-line decisions when obesity, heart failure, chronic kidney disease, or cardiovascular disease are major factors.
There is no single universally safer alternative. The right alternative depends on kidney function, side effects, cost, weight goals, heart disease, heart failure, chronic kidney disease, and risk of low blood sugar. That is why medication choice should be individualized rather than copied from a generic list.
There is no single A1C number that automatically means “start metformin” for every patient. Metformin is a common first-line medication once type 2 diabetes is diagnosed, but the full decision depends on the overall clinical picture. What is clearer in current ADA standards is that insulin should be considered when A1C is above 10% or blood glucose is 300 mg/dL or higher, especially if symptoms are present.
They can, but portion size and context matter. Refined crackers are usually more likely to raise blood sugar quickly than higher-fiber choices, especially if eaten alone. A more blood-sugar-friendly approach is to keep portions modest and pair crackers with protein or fat, such as cheese, peanut butter, or hummus. That is a practical inference from CDC’s healthy eating and meal-planning guidance.
The better choice is usually toast with more fiber and less added sugar, eaten in a sensible portion and paired with protein. Whole-grain or seeded breads are often a better fit than refined white bread for many patients, though the overall meal pattern matters more than a single slice of toast. That answer aligns with the CDC’s overall advice to focus on healthy foods, portion sizes, and timing rather than rigid food bans.
There is no single universal “worst” food for every patient. In practice, sugar-sweetened drinks and easy-to-overeat refined carbs often cause the least helpful blood sugar patterns because they deliver a lot of fast carbohydrate with little fiber or fullness. A better approach is to think in patterns, not villain foods.
Remission is possible for some patients, especially with significant weight loss, but it is not guaranteed and it is not the same as a cure. Large weight loss, including after metabolic surgery in selected patients, can lead to remission in some cases.
A PDF can be useful as a reference, but it should not replace a personal treatment plan. Diabetes care needs to match the patient’s A1C, glucose pattern, kidney function, weight, medications, and complication risk. For a clinic website, the stronger offer is a doctor-guided care plan rather than a one-size-fits-all handout.
That is one reason so many people live with it before they fully understand what is happening. CDC says type 2 diabetes symptoms often develop over several years, and some people do not notice any symptoms at all.
That slow start can be misleading. Type 2 diabetes is still a serious condition. It raises the risk of heart disease, kidney disease, vision loss, nerve damage, and foot problems when it is not well managed. The good news is that modern type 2 diabetes management is far more flexible and effective than many patients expect. Treatment is no longer just “take a pill and avoid sugar.” Good care now combines lifestyle changes, glucose monitoring, and medication choices based on the patient’s blood sugar, weight, kidney function, heart risk, and daily routine.
What Type 2 Diabetes Is
Type 2 diabetes is the most common form of diabetes. CDC says more than 40 million Americans have diabetes, about 90% to 95% of them have type 2 diabetes, and the condition usually develops in adults but is also appearing more often in children, teens, and young adults.
How insulin resistance develops
In type 2 diabetes, the body does not use insulin well. This is called insulin resistance. At first, the pancreas tries to keep up by making more insulin. Over time, it cannot keep pace, and blood sugar rises. CDC describes insulin as the “key” that helps blood sugar enter cells for energy and explains that in type 2 diabetes, cells stop responding normally to it.
What Causes Type 2 Diabetes
There is no single cause. Type 2 diabetes develops from a mix of metabolic, genetic, and lifestyle factors. NIDDK lists overweight or obesity, physical inactivity, insulin resistance, and genes as major contributors. CDC adds that risk is higher with prediabetes, age 45 or older, family history, history of gestational diabetes, and certain racial and ethnic backgrounds in the U.S.
Main risk factors
The biggest risk factors are familiar but still important: excess body weight, especially when combined with low physical activity; family history; prediabetes; prior gestational diabetes; and related conditions such as high blood pressure or fatty liver disease. None of these factors means diabetes is inevitable, but together they raise the odds significantly.
What patients often misunderstand
Patients often think type 2 diabetes is only about sugar intake. It is broader than that. Food matters, but so do body weight, activity, genetics, sleep, liver health, insulin resistance, and how the body handles glucose over time. That is why good treatment is not built around one food rule or one lab number. It is built around the whole patient.
Symptoms of Type 2 Diabetes
Common symptoms include increased thirst, frequent urination, increased hunger, fatigue, blurred vision, numbness or tingling in the hands or feet, sores that do not heal, and sometimes unexplained weight loss. NIDDK notes that symptoms of type 2 diabetes often develop slowly over several years and may be so mild that people do not notice them.
Common early symptoms
A patient may notice that they are thirstier than usual, more tired than they should be, or waking up more often to urinate. Others first notice blurred vision, tingling in the feet, or skin or wound-healing issues. These signs are easy to minimize at first. Still, when they cluster together, they should prompt testing.
Why many people miss the signs
Type 2 diabetes can stay quiet for a long time. CDC says some people have no noticeable symptoms at all. Others only learn they have diabetes after a routine blood test or after a complication begins to show up. That is one reason routine screening and risk-based testing matter, especially for adults with risk factors.
How to Diagnose Type 2 Diabetes
Doctors diagnose type 2 diabetes with blood tests, not guesswork. NIDDK lists the four main diagnostic tests as the A1C test, fasting plasma glucose test, oral glucose tolerance test, and random plasma glucose test when symptoms are present.
Blood tests used to diagnose type 2 diabetes
According to NIDDK, diabetes is diagnosed at:
- A1C: 6.5% or above
- Fasting plasma glucose: 126 mg/dL or above
- 2-hour oral glucose tolerance test: 200 mg/dL or above
- Random plasma glucose: 200 mg/dL or above when symptoms are present.
What the results mean
Those numbers confirm diabetes, but the diagnosis is only the start. Once the diagnosis is made, the next step is deciding how aggressive treatment needs to be and whether there are already related issues such as kidney disease, hypertension, cholesterol problems, or symptoms of high blood sugar that need attention right away.
Type 2 Diabetes Management Guidelines: What Modern Care Includes
Modern type 2 diabetes management guidelines are not built around blood sugar alone. NIDDK’s diabetes management guidance emphasizes the “ABCs” of care: A1C, blood pressure, and cholesterol, along with smoking cessation, medicines, and a realistic care plan.
Lifestyle treatment
Lifestyle treatment is the base layer of care. CDC and NIDDK both stress healthy eating, regular physical activity, weight management, and keeping follow-up appointments. For people with overweight or obesity, even modest weight loss can help. NIDDK’s prevention guidance says losing 5% to 10% of current body weight can help reduce risk, and ADA’s 2026 standards note that in type 2 diabetes with overweight or obesity, medications that lower glucose and support weight loss are preferred when appropriate.
Blood sugar, blood pressure, and cholesterol
This is where many patients need a reset. Good diabetes care is not just about glucose. NIDDK says that managing blood glucose, blood pressure, and cholesterol is central to lowering the chances of heart attack, stroke, kidney disease, blindness, and amputations. That is why treatment plans often include blood pressure medicine, statins, kidney protection, or smoking cessation support in addition to glucose-lowering medication.
Monitoring and follow-up
Monitoring matters because treatment should change when the numbers change. NIDDK says many people with diabetes aim for an A1C below 7%, though goals should be individualized. For many patients, blood sugar targets are 80 to 130 mg/dL before meals and less than 180 mg/dL about two hours after a meal starts. If a patient uses CGM, NIDDK says the usual target range is 70 to 180 mg/dL and many aim to stay in range at least 70% of the time.
First-Line Treatment for Diabetes Type 2
The phrase first-line treatment for diabetes type 2 sounds simple, but the real answer is more nuanced now.
Metformin and when it fits
ADA’s 2026 pharmacologic standards say metformin is a commonly used medication that historically has been the first-line treatment for type 2 diabetes. It remains a strong option because it is effective, familiar, and generally low risk for hypoglycemia. Still, it is no longer the only starting point in every patient. Doctors now personalize treatment earlier based on obesity, cardiovascular disease, heart failure, kidney disease, side effects, and cost.
Diabetes type 2 medications list: what doctors may choose next
A diabetes type 2 medications list can include metformin, GLP-1 receptor agonists, dual GIP/GLP-1 medicines, SGLT2 inhibitors, DPP-4 inhibitors, sulfonylureas, thiazolidinediones, and insulin. The “best” option depends on the patient. ADA’s 2026 standards note that in people with type 2 diabetes and overweight or obesity, agents with both glucose-lowering and weight-loss effects are preferred, and in people with chronic kidney disease, SGLT2 inhibitors are recommended at eGFR ≥20 mL/min/1.73 m² because they slow CKD progression and reduce heart failure risk.
That is why there is no single best medicine for diabetes type 2 for everyone. There is only the best medication choice for a specific patient at a specific point in time. The same logic applies to the search phrase best medicine for type 2 diabetes without side effects: no medicine is truly side-effect-free. Good prescribing is about balancing benefit, safety, cost, and fit
When insulin may be needed
Insulin is not reserved only for late disease. ADA’s 2026 standards say clinicians should consider insulin as the first injectable when symptoms of hyperglycemia are present or when blood sugar is very high, such as A1C above 10% or blood glucose 300 mg/dL or higher. In practice, that means a patient with significant symptoms, marked weight loss, or very high glucose may need faster treatment than pills alone can provide.
Just Diagnosed With Type 2 Diabetes: What Can I Eat?
This is one of the first questions patients ask, and for good reason. Food feels personal. It also feels immediate. CDC’s healthy eating guidance says the goal is to eat healthy foods in the right amounts at the right times so blood sugar stays in target as much as possible. It also recommends working with a dietitian or diabetes educator on a practical meal plan.
What to build meals around
If you are just diagnosed with type 2 diabetes, start with a simple framework: build more meals around vegetables, lean protein, beans, lentils, eggs, fish, chicken, yogurt without added sugar, nuts, and higher-fiber carbohydrate choices. CDC’s current nutrition guidance emphasizes whole, nutrient-dense foods, including vegetables, fruits, protein foods, healthy fats, and whole grains.
What to limit
Limit sugar-sweetened drinks, oversized portions, and frequent refined starches that are easy to overeat. That does not mean a person with diabetes can never eat crackers or toast again. It means refined crackers and white toast are usually tougher on blood sugar than higher-fiber options, especially when eaten alone. A practical inference from CDC’s healthy eating guidance is to choose smaller portions, pair carbohydrates with protein or fat, and favor higher-fiber choices more often than ultra-refined ones.
Type 2 Diabetes Blood Sugar and Urine Sugar Levels
Blood glucose testing remains the main way to monitor type 2 diabetes. For many adults with diabetes, common targets are 80–130 mg/dL before meals and less than 180 mg/dL about two hours after a meal starts. For people using a CGM, the usual target range is often 70–180 mg/dL. Still, targets can vary, so patients should follow the plan set by their doctor.
Urine sugar testing can still be useful as a supporting check. However, it is less accurate than blood glucose testing for diagnosing and monitoring diabetes day to day. The urine glucose testing was used more often in the past, but blood tests are now more commonly used because they are more accurate.
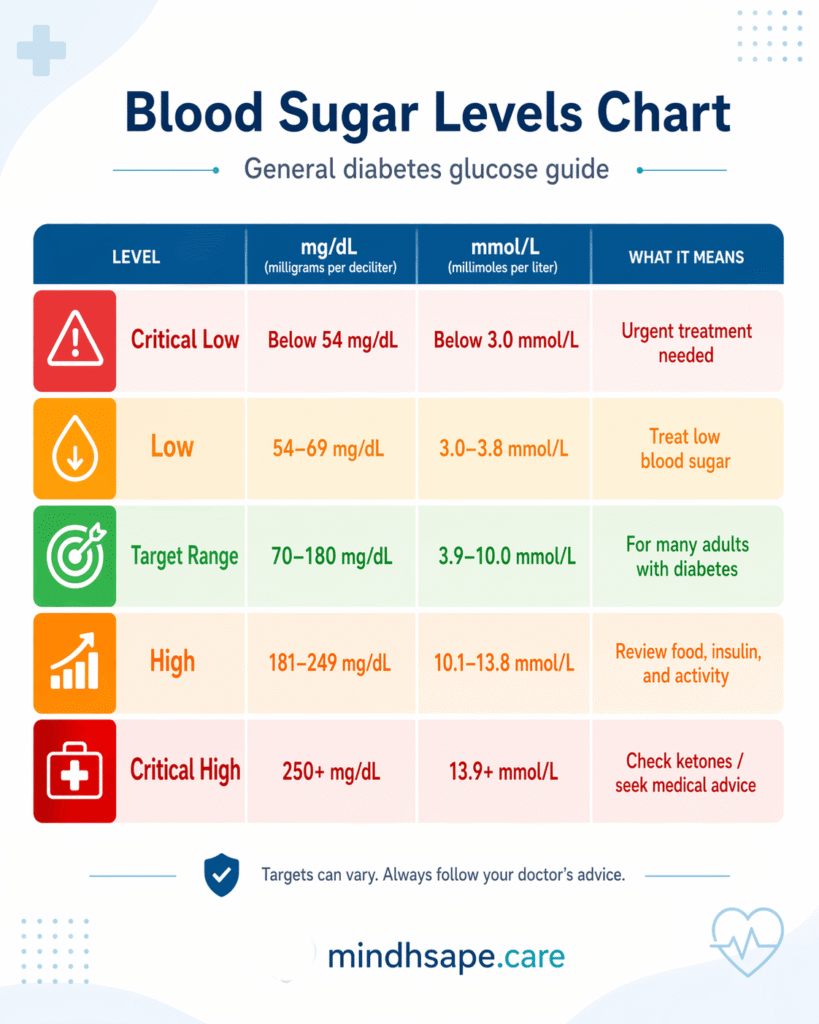
What Level of Blood Sugar Is Dangerous for Type 2 Diabetes?
For most people, below 70 mg/dL is too low and above 180 mg/dL is too high. During illness, blood sugar needs even closer attention. If blood sugar rises above 240 mg/dL, ketone testing may be needed. If it stays very high, especially around 300 mg/dL or more with worsening symptoms, medical advice should not be delayed.
Urine Sugar Levels Chart for Type 2 Diabetes Management
A urine sugar chart can help patients understand what a positive dipstick result may suggest. Even so, it should be treated as a supportive guide, not the main method of diabetes monitoring. Most urine dipstick tests report results as negative, trace, 1+, 2+, 3+, or 4+ instead of giving the kind of direct value patients get from a blood glucose meter.
The chart below gives a simple visual guide to urine sugar levels and what they may mean in type 2 diabetes management.
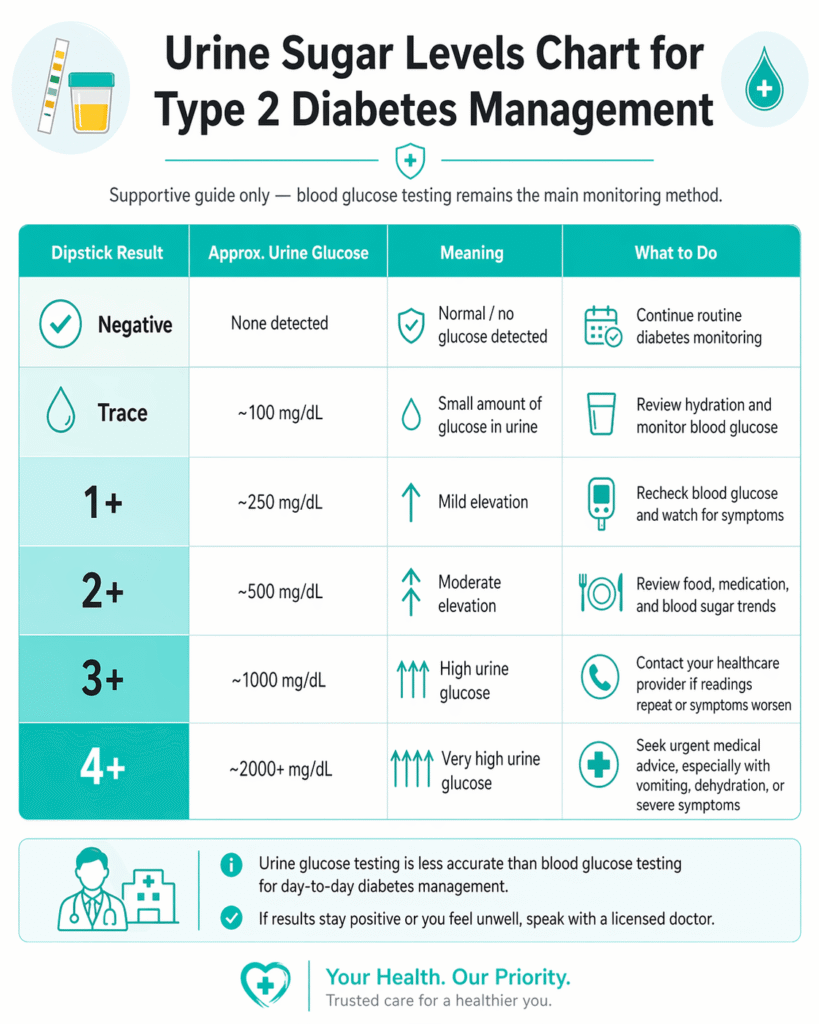
For daily treatment decisions, patients should rely on blood glucose monitoring and follow the targets set by their doctor.
In general, a negative result means no glucose was detected in the urine. A trace result suggests a small amount. On many dipstick scales, trace is about 100 mg/dL, 1+ about 250 mg/dL, 2+ about 500 mg/dL, 3+ about 1000 mg/dL, and 4+ about 2000 mg/dL or higher. These are approximate urine glucose categories and may vary by strip brand and testing method.
For patients with type 2 diabetes, repeated positive urine sugar readings may suggest that blood sugar has been elevated for some time. Still, urine glucose can be influenced by other factors, and some people may have glucose in the urine for reasons other than diabetes. That is why doctors rely more on blood glucose testing when making treatment decisions.
If urine sugar stays positive, symptoms worsen, or the patient feels unwell, it is best to contact a licensed doctor promptly. In addition, urgent care is needed if very high sugar levels are paired with vomiting, dehydration, breathing trouble, or severe weakness.
Type 2 Diabetes Complications
Type 2 diabetes complications are the reason steady treatment matters. NIDDK lists heart disease, stroke, nerve damage, kidney disease, foot problems, eye disease, gum disease, sexual and bladder problems, and fatty liver disease among the major risks. CDC’s current diabetes report card also highlights blindness, kidney failure, heart disease, stroke, and limb loss as major risks.
This is not meant to scare patients. It is meant to clarify the goal. Good management is about more than lowering one lab value. It is about protecting vision, kidneys, nerves, feet, heart, and quality of life over the long term.
Can You Reverse Type 2 Diabetes at Any Stage?
The most careful medical word here is remission, not cure. CDC says there is not yet a cure for diabetes. However, remission can happen in some people with type 2 diabetes, especially after substantial weight loss. NIDDK’s weight-management guidance notes that with larger amounts of weight loss, such as after bariatric surgery, remission of type 2 diabetes can occur in some patients. ADA’s 2026 obesity standards also state that metabolic surgery often leads to remission.
So, can you reverse type 2 diabetes at any stage? Sometimes people can reach remission, particularly earlier in the disease course and especially with major weight loss, but it is not guaranteed, and it does not mean long-term follow-up can stop. For a clinic website, the safest wording is this: remission is possible for some patients, but it should be pursued through a medically supervised plan, not internet promises.
Final Thoughts on Type 2 Diabetes Management
Good type 2 diabetes management is not about one food, one number, or one prescription. It is a care plan. That plan usually includes healthier eating, physical activity, weight management, glucose monitoring when needed, and medication chosen for the patient’s real risks and real life. For many people, the right plan also includes blood pressure control, cholesterol treatment, kidney protection, and regular eye and foot care.
The best results usually come from early action. If symptoms are showing up, if lab work is drifting, or if treatment no longer feels clear, that is the time to reassess the plan with a licensed clinician. Type 2 diabetes is common. It is serious. And with the right treatment strategy, it is manageable.
Ready to get online type 2 diabetes management?
Book an appointment with a licensed doctor for diabetes evaluation, medication review, blood sugar assessment, and a personalized type 2 diabetes management or care plan.
If you have already been diagnosed, our clinical team can help you understand treatment options, insulin routines, blood sugar patterns, and next-step management.
A caring note from MindShape Care
This article is for education only and is not a diagnosis. If your symptoms feel severe, urgent, or unsafe, please seek immediate emergency or crisis support.
This article was reviewed and written with insights from the Medical team at Medically reviewed by licensed clinicians at mindhsape.care. in the USA — experienced healthcare professionals specializing in anxiety, depression, chronic kidney disease, all types of diabetes, hair loss, hormonal health, hyperlipidemia, hypertension, low testosterone, nutrition management, obesity, obstructive sleep apnea, PCOS, and infertility, and patient wellness. Learn more about our board-certified doctors and treatment experts who contribute to our educational blogs and patient support programs.
Recent Blogs
Learn more about Virtual Healthcare and Treatments
Why You Can Rely on Us?
At Mindshape Clinic, we are committed to providing clear and trustworthy health information that you can rely on.
Reliable Information – Every article is based on credible sources.
Expert Review – Content is carefully checked before publishing.
Up to Date – We keep information current with the latest insights.
Clarity First – Our goal is to make knowledge simple and accessible.